Monkeypox is a rare, but potentially serious viral disease that is caused by the monkeypox virus. The disease was first discovered in 1958, when outbreaks of a pox-like disease occurred in monkeys kept for research. The first human case was reported in 1970 in the Democratic Republic of Congo, and since then, cases have been reported in several African countries. In 2003, the first cases of monkeypox were reported outside of Africa, in the United States, following an outbreak that was traced to imported African rodents.
Monkeypox is similar to human smallpox, but it is less severe. The disease is usually self-limiting, meaning that it will resolve on its own without treatment. However, in some cases, monkeypox can be severe and even fatal. The disease is transmitted to humans through contact with the blood, bodily fluids, or skin lesions of infected animals, or through contact with contaminated objects, such as bedding or clothing. Human-to-human transmission of monkeypox is also possible, but it is generally less efficient than animal-to-human transmission.
Key Takeaways
- Monkeypox is a viral disease that is caused by the monkeypox virus, and is similar to human smallpox.
- The disease is usually self-limiting, but can be severe and even fatal in some cases.
- Monkeypox is transmitted to humans through contact with infected animals or contaminated objects, and human-to-human transmission is possible but less efficient.
Overview of Monkey Pox
Monkeypox is an infectious disease caused by the monkeypox virus. The virus is a member of the Orthopoxvirus genus, which also includes the smallpox virus. Monkeypox was first identified in 1958 when outbreaks of a pox-like disease occurred in monkeys kept for research. The first human case was reported in 1970 in the Democratic Republic of Congo.
Symptoms
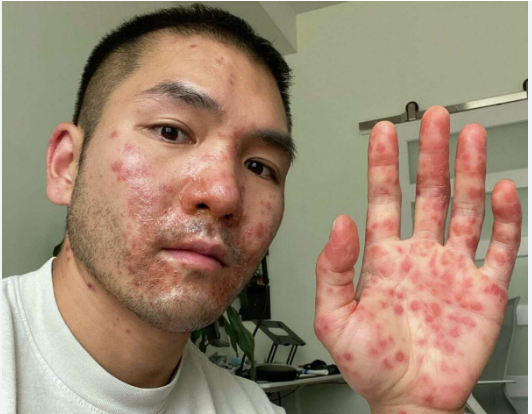
The symptoms of monkeypox are similar to those of smallpox, but milder. The incubation period is usually 5-14 days. The first symptoms are fever, headache, muscle aches, and backache. A rash then develops, often beginning on the face and then spreading to other parts of the body. The rash changes and goes through different stages before finally forming a scab, which later falls off.
Transmission
Monkeypox is primarily a zoonotic disease, meaning it is transmitted from animals to humans. The virus is believed to be transmitted to humans through contact with infected animals, such as monkeys, rodents, and rabbits. Human-to-human transmission is also possible, primarily through respiratory droplets or contact with bodily fluids of infected individuals.
Prevalence
Monkeypox is endemic in Central and West African countries, including Cameroon, Central African Republic, Democratic Republic of Congo, Liberia, Nigeria, and Sierra Leone. Outbreaks have also occurred outside of Africa, such as in the United States, where there have been a few cases reported in recent years. Monkeypox is a rare disease, and the risk of contracting the virus is low for most people. However, individuals who come into close contact with infected animals or humans are at higher risk.
Historical Background of Monkey Pox
Monkeypox is a viral disease that was first identified in monkeys in 1958. The virus was later found to infect humans in 1970 when an outbreak occurred in the Democratic Republic of Congo. The disease is caused by the monkeypox virus, which is a member of the Orthopoxvirus genus, the same family as smallpox.
Monkeypox’s past is intertwined with that of smallpox, which is believed to have first appeared around 10,000 B.C.E. Smallpox was one of humanity’s deadliest diseases, killing more than 300 million people in the 20th century alone. The eradication of smallpox in 1980 was a major achievement in global health, and the success of the smallpox eradication campaign has provided a model for other disease control efforts.
Monkeypox is endemic in Central and West African countries, where it is transmitted to humans from animals such as rodents and primates. The disease is typically self-limiting, with symptoms including fever, headache, muscle aches, and rash. However, severe cases can lead to complications such as pneumonia, encephalitis, and death.
The first case of monkeypox outside of Africa was reported in the United States in 2003, and since then, there have been sporadic outbreaks in other parts of the world. In 2022, monkeypox broke through in Africa, America, Eastern Mediterranean, Europe, South-East Asia, and Western Pacific region. The emergence of monkeypox in new areas highlights the need for continued surveillance and research to better understand the disease and prevent its spread.
In conclusion, monkeypox has a rich history, intertwined with that of smallpox. While the disease is typically self-limiting, severe cases can lead to complications and death. The emergence of monkeypox in new areas underscores the importance of continued research and surveillance to prevent its spread.
Diagnosis and Testing of Monkey Pox
Monkeypox is a rare viral disease that is difficult to diagnose clinically because of its similarity to other diseases such as smallpox, chickenpox, and measles. Therefore, laboratory testing is essential for confirming the diagnosis of monkeypox.
Laboratory Testing
Laboratory testing for monkeypox includes the detection of viral DNA or antigens in clinical specimens, such as blood, serum, pus, or tissue samples. The most commonly used tests are polymerase chain reaction (PCR) and enzyme-linked immunosorbent assay (ELISA). PCR is a highly sensitive and specific test that can detect the virus within a few days of infection, while ELISA can detect the presence of antibodies against the virus in the blood.
Another test that can be used for the diagnosis of monkeypox is virus isolation, which involves growing the virus in cell culture from clinical specimens. However, this test is time-consuming and requires specialized laboratory facilities.
Clinical Diagnosis
Clinical diagnosis of monkeypox is based on the presence of characteristic symptoms, such as fever, headache, muscle aches, backache, swollen lymph nodes, and a rash that progresses from macules to papules to vesicles to pustules. The rash typically appears on the face, trunk, and limbs, including the palms and soles of the feet.
However, the clinical presentation of monkeypox can vary widely, and some cases may not present with a rash. Therefore, a thorough medical history, including recent travel to endemic areas and exposure to animals, is essential for making a clinical diagnosis of monkeypox.
In conclusion, laboratory testing and clinical diagnosis are both important for the accurate diagnosis of monkeypox. Clinicians should be aware of the clinical presentation of monkeypox and consider the possibility of the disease in patients with a compatible clinical syndrome, especially those with a history of travel to endemic areas or exposure to animals.
Treatment and Prevention
Monkeypox is a rare disease caused by the monkeypox virus. There is no specific treatment for monkeypox, but supportive care can help manage symptoms and prevent complications.
Medications
Antiviral medications, such as tecovirimat, may be used to treat severe cases of monkeypox. These medications work by preventing the virus from replicating in the body. However, their effectiveness is still being studied.
Vaccines
The JYNNEOS vaccine has been approved by the FDA for the prevention of monkeypox in adults. It is recommended for people who are at high risk of exposure to the virus, such as laboratory workers, animal handlers, and healthcare workers. The vaccine is also recommended for travelers to areas where monkeypox is endemic.
Preventive Measures
Preventive measures can help reduce the risk of monkeypox infection. These include:
- Avoiding contact with animals that may carry the virus, such as rodents and primates.
- Washing hands frequently with soap and water.
- Using personal protective equipment, such as gloves and masks, when handling animals or animal products.
- Quarantining infected individuals to prevent the spread of the virus.
It is important to note that monkeypox is a rare disease, and the risk of infection is low for most people. However, it is still important to take precautions to protect yourself and others from the virus.
Impact on Public Health
Monkeypox has a significant impact on public health due to its highly contagious nature and potential to cause severe illness. The disease can be transmitted from animals to humans through direct contact with infected animals or through the consumption of contaminated meat. It can also be transmitted from person to person through respiratory droplets or contact with bodily fluids.
The symptoms of monkeypox include fever, headache, muscle aches, backache, swollen lymph nodes, chills, and exhaustion. A rash then develops, often beginning on the face and then spreading to other parts of the body. In severe cases, the rash can become pustular and cause scarring.
Due to the severity of the disease, monkeypox outbreaks have the potential to overwhelm healthcare systems and put a strain on resources. Moreover, the disease can be difficult to diagnose, as the symptoms are similar to those of other viral illnesses such as chickenpox and smallpox.
Prevention measures such as vaccination, quarantine, and public health education campaigns are essential to controlling the spread of monkeypox. Vaccination is particularly important for those who are at high risk of exposure, such as healthcare workers and veterinarians. Additionally, early detection and prompt treatment of cases can help to reduce the severity of the disease and prevent further transmission.
In conclusion, monkeypox has a significant impact on public health due to its highly contagious nature and potential to cause severe illness. Prevention measures such as vaccination and public health education campaigns are essential to controlling the spread of the disease.
Current Research and Developments
Vaccine Development
Monkeypox is a rare but potentially deadly disease caused by the monkeypox virus. With no specific treatment available, vaccination is the best way to prevent the spread of this disease. Currently, there are two vaccines available for monkeypox: the first-generation vaccine and the second-generation vaccine.
The first-generation vaccine is a live-virus vaccine that was developed in the 1960s and provides immunity against monkeypox and smallpox. However, it has several limitations, including the risk of severe side effects in people with weakened immune systems. Therefore, the second-generation vaccine was developed, which is a non-replicating vaccine that does not contain live virus particles. The second-generation vaccine is safer and provides better protection against monkeypox than the first-generation vaccine.
Recently, the White House Office of Science and Technology Policy published the U.S. Monkeypox Research Priorities to speed up the development of a safer and more effective vaccine. The research priorities include developing a next-generation vaccine that is safe for immunocompromised individuals and can provide long-lasting protection against monkeypox.
Treatment Research
There is currently no specific treatment available for monkeypox. However, several antiviral drugs have shown promise in treating monkeypox in animal models. One of these drugs is cidofovir, which has been used to treat monkeypox in humans on a case-by-case basis. Another drug, brincidofovir, is currently being evaluated in clinical trials for its effectiveness against monkeypox.
In addition to antiviral drugs, monoclonal antibodies are being developed as a potential treatment for monkeypox. Monoclonal antibodies are laboratory-produced molecules that can mimic the immune system’s ability to fight off viruses. They have shown promise in treating other viral diseases such as Ebola and COVID-19.
Overall, there is ongoing research and development in the field of monkeypox, with a focus on developing safer and more effective vaccines and treatments. The research priorities set by the White House Office of Science and Technology Policy are expected to accelerate the development of these interventions, which will be crucial in controlling future outbreaks of monkeypox.
Conclusion
Monkeypox is a viral disease that can be transmitted from animals to humans. The virus causes a range of symptoms, including fever, headache, muscle aches, and rash. While monkeypox is generally a self-limiting disease, it can be severe in some cases.
The recent outbreak of monkeypox in 2022 highlights the need for improved surveillance and detailed monitoring of the virus. The outbreak affected 16 countries, with 528 infections diagnosed between April and June. The majority of those infected were gay or bisexual men, and 75% were White [1].
The virus is primarily transmitted through contact with infected animals, but it can also be passed from person to person through respiratory droplets or contact with bodily fluids. In addition to humans, monkeypox has been found in a variety of animals, including rodents, primates, and squirrels [2].
Prevention and control measures for monkeypox include vaccination, use of personal protective equipment, and proper hygiene practices. Vaccination is the most effective way to prevent monkeypox, and it is recommended for people who are at high risk of exposure to the virus, such as healthcare workers and laboratory staff [3].
In conclusion, monkeypox is a serious disease that requires ongoing monitoring and control measures to prevent outbreaks and protect public health. While the recent outbreak is concerning, it also highlights the importance of preparedness and response efforts to address emerging infectious diseases.
Frequently Asked Questions
What are the first signs of monkeypox?
The first signs of monkeypox usually appear within 5 to 21 days after exposure to the virus. The initial symptoms are similar to flu-like symptoms, including fever, headache, muscle aches, backache, swollen lymph nodes, chills, and exhaustion. A rash then appears, often beginning on the face then spreading to the trunk and limbs. The rash develops into raised bumps that fill with fluid and then crust over.
Is monkeypox contagious?
Yes, monkeypox is contagious. The virus can be spread through contact with bodily fluids, such as blood, saliva, or respiratory secretions, of an infected person or animal. It can also be spread by touching objects contaminated with the virus, such as bedding or clothing.
Is monkeypox deadly?
Monkeypox can be deadly, but it is usually a self-limited disease that does not require treatment. The mortality rate for monkeypox is generally low, ranging from 1% to 10% in Africa, where the disease is endemic. However, in rare cases, monkeypox can cause severe illness and death in people with weakened immune systems.
How is monkeypox transmitted?
Monkeypox is transmitted through contact with bodily fluids or contaminated objects. The virus can be spread through close contact with an infected person or animal, such as touching or caring for them. It can also be spread through respiratory droplets, such as when an infected person coughs or sneezes.
Is there a cure for monkeypox?
There is no specific treatment or cure for monkeypox. However, supportive care can help manage symptoms and prevent complications. Antiviral drugs and vaccines are being developed, but their efficacy has not been fully established.
Monkeypox prevention
Preventing monkeypox involves avoiding contact with infected animals and people. Avoiding contact with wild animals, such as rodents and primates, and practicing good hygiene, such as washing hands frequently and avoiding touching objects that may be contaminated, can help reduce the risk of infection. Vaccination is also available for people at high risk of exposure, such as healthcare workers and laboratory personnel.
Also read:








Leave a Reply
View Comments